What to Do After an Accident
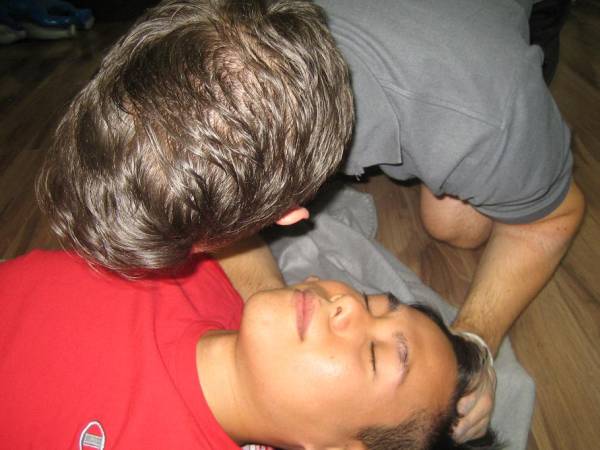
If someone is injured in an incident, first check that you and the casualty are not in any danger. If you are, make the situation safe. When it’s safe to do so, assess the casualty and call for an ambulance (if necessary). You can then carry out basic first aid. Assessing a casualty The priorities […]
Unconsciousness
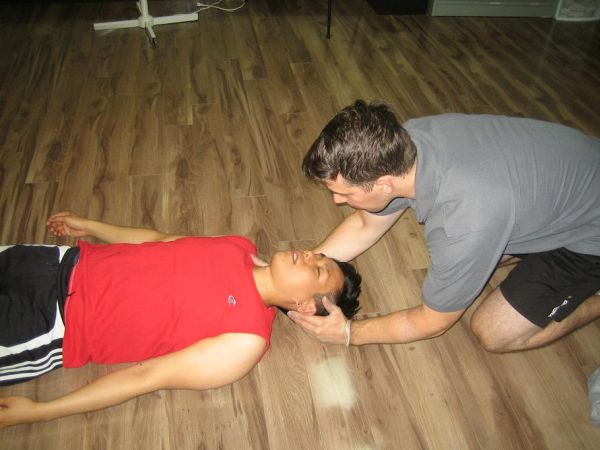
Unconsciousness is when a person suddenly becomes unable to respond to stimuli and appears to be asleep. A person may be unconscious for a few seconds (fainting) or for longer periods of time. People who become unconscious don’t respond to loud sounds or shaking. They may even stop breathing or their pulse may become faint. […]
Travel First Aid
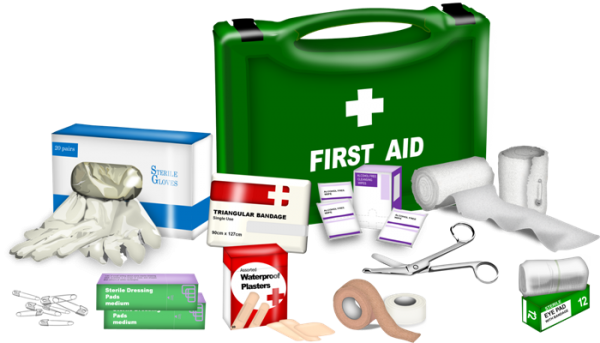
Travel First Aid Kit Just as you prepare first aid kits for your home and car, you should also create one for travel. Your travel kit can be customized for every trip. You will want to bring basic supplies found in your standard home emergency kit, but you should also include other items. Consider the […]
Snake Bites

What Are Snake Bites? A bite from a venomous snake can be deadly, and should always be treated as a medical emergency. Even a bite from a harmless snake can be serious, leading to an allergic reaction or an infection. Venomous snake bites can produce an array of symptoms, including localized pain and swelling, convulsions, […]
Shock

Lay the Person Down, if Possible Elevate the person’s feet about 12 inches unless head, neck, or back is injured or you suspect broken hip or leg bones. Do not raise the person’s head. Turn the person on side if he or she is vomiting or bleeding from the mouth. Begin CPR, if Necessary If the person […]
Poisoning First Aid

Poisoning is injury or death due to swallowing, inhaling, touching or injecting various drugs, chemicals, venoms or gases. Many substances such as drugs and carbon monoxide are poisonous only in higher concentrations or dosages. And others such as cleaners are dangerous only if ingested. Children are particularly sensitive to even small amounts of certain drugs […]
Nose Bleeds
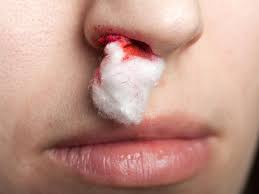
Stop the Bleeding Have the person sit up straight and lean forward slightly. Don’t have the person lie down or tilt the head backward. With thumb and index finger, firmly pinch the nose just below the bone up against the face. Apply pressure for 5 minutes. Time yourself with a clock. If bleeding continues after […]
Muscles Strains
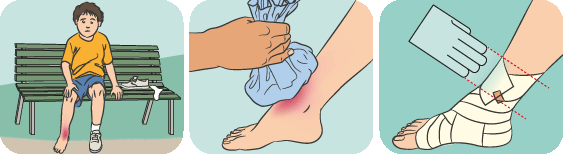
Control Swelling and Prevent Further Injury With PRICE Protect by applying an elastic bandage, sling, or splint. Rest the muscle for at least a day. Ice immediately, and continue to ice for 10 to 15 minutes every hour, for 2-3 days. Compress by gently wrapping with an Ace or other elastic bandage. (Don’t wrap tightly.) Elevate injured area […]
Motion Sickness

Any type of transportation can cause motion sickness. It can strike suddenly, progressing from a feeling of uneasiness to a cold sweat, dizziness and then vomiting. Motion sickness usually quiets down as soon as the motion stops. The more you travel, the more easily you’ll adjust to being in motion. You may escape motion sickness […]
Minor Cut Management
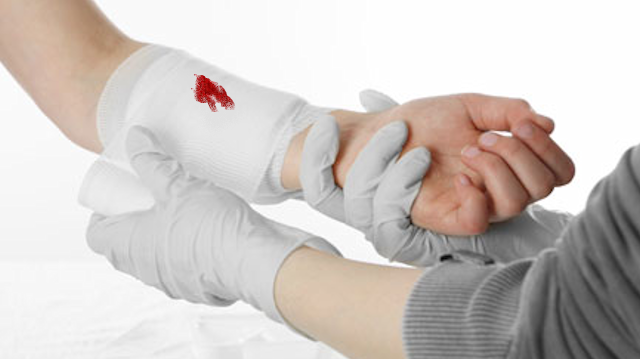
Minor cuts and scrapes usually don’t require a trip to the emergency room. These guidelines can help you care for such wounds: Wash your hands. This helps avoid infection. Also put on disposable protective gloves if they’re available. Stop the bleeding. Minor cuts and scrapes usually stop bleeding on their own. If not, apply […]
